Treating Friedreich’s ataxia
From diagnosis to ongoing management, treating Friedreich’s ataxia (FA) is a community effort.
From diagnosis to ongoing management, treating Friedreich’s ataxia (FA) is a community effort.
Diagnosing FA as early as possible is critical due to the progressive nature of the disease. Studies have shown that individuals younger than the age of 18 years progress faster than those with intermediate to late onset.1,2
The diagnostic journey may begin with a primary care doctor or pediatrician performing assessments to check your balance, sensations, reflexes, and more. If their suspicion of FA grows stronger, they may refer you to a series of specialists who can conduct additional tests such as3
Electromyogram (EMG) – Measures the electrical activity of muscle cells
Nerve conduction studies – Measures the speed with which nerves transmit impulses
Electrocardiogram (ECG) – Provides a graphic presentation of the electrical activity or beat pattern of the heart
Echocardiogram – Records the motion and function of the heart muscle
Blood test – Checks for elevated glucose and vitamin E levels seen in FA
Magnetic resonance imaging (MRI) or computed tomography (CT) scans – Provides images of the brain and spinal cord
Your doctor should order a genetic test to confirm their suspicions. A genetic test will determine if the mutated gene that leads to frataxin deficiency, the root cause of FA, is present.3 It will also identify the number of GAA repeats, which may give insight into how the disease could progress over time.4
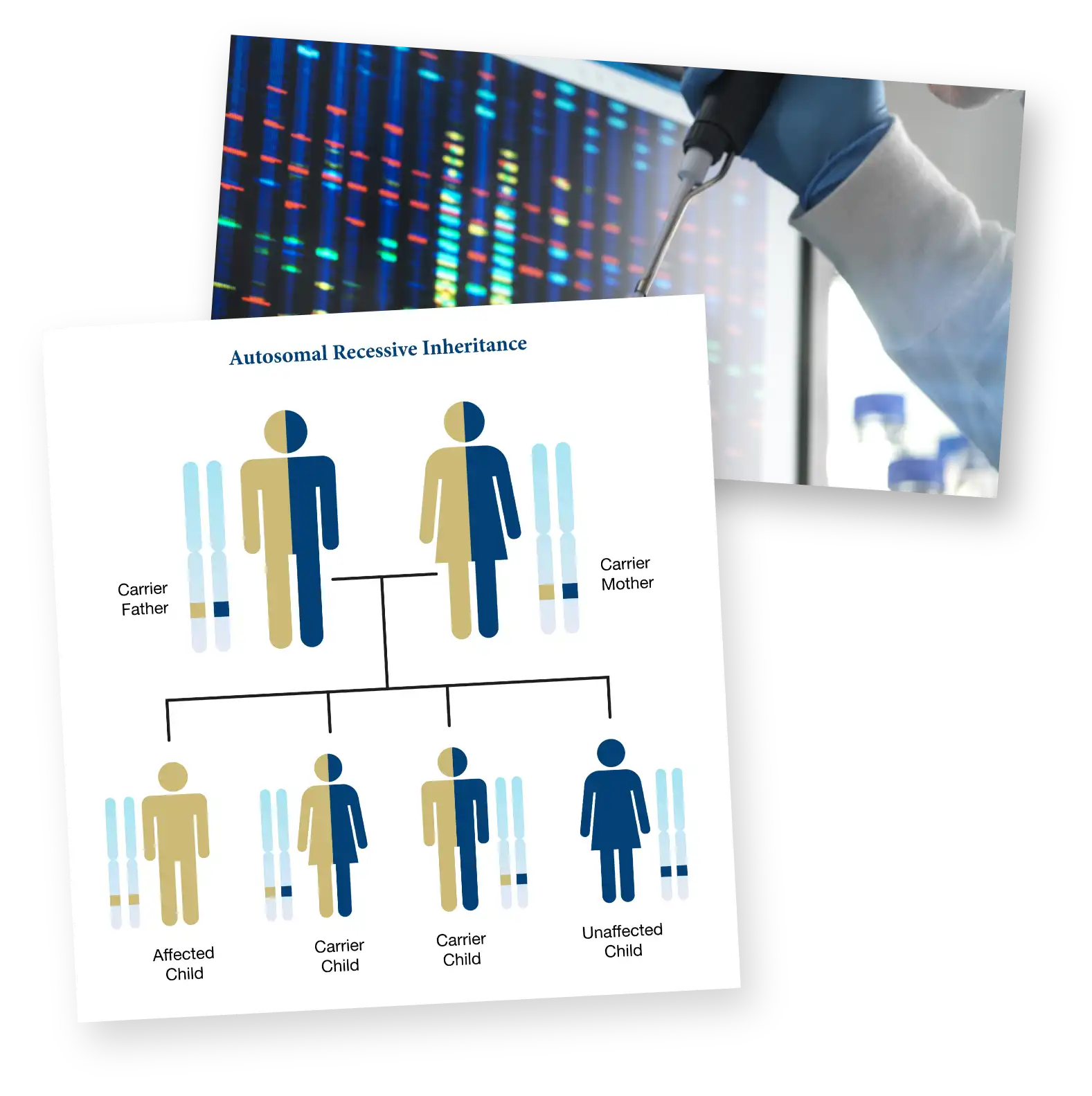
In order to be affected by FA, you have to inherit 2 mutated genes, 1 from each parent. If you inherit only 1 copy of the mutated gene, you are considered a carrier. A carrier will not develop FA but can pass on the mutated gene to their children. If 2 carriers have children, each child has a 25% chance of developing FA.3,5
A genetic counselor can help you and your family better understand how FA is inherited and if other family members could be affected.5
Managing FA involves treatment with medication and different forms of therapy, including physical, occupational, speech, and language. In some cases, surgery is required, as well as addressing any related complications, such as diabetes or heart conditions.1,3
Upright stability assessment
9-hole peg test
Timed 25-foot walk test
Patient-reported outcomes (PROs), such as Friedreich Ataxia Rating Scale-Activities of Daily Living (FARS-ADL), Modified Fatigue Impact Scale, etc.
Research is ongoing to help develop treatments that address the root cause of the disease—frataxin deficiency—and not just its symptoms.4
In a national survey of 50 physicians who treat patients with FA: 94% agree there are still patient needs that are not being met in FA treatment.8
In a national survey of 50 physicians who treat patients with FA: 98% believe there is a need for a treatment that targets frataxia levels directly.8
Due to the multisystem nature of the disease, managing FA often requires a variety of providers and specialists. If you’re currently seeing a primary care provider, finding an FA expert could be helpful to receive more specialized care. Along your journey, you may encounter the following types of doctors9:
No one FA journey will be the same, so each person’s care team might look different.9
Neurologists
assess and manage your symptoms related to ataxia and neurologic function
A primary care provider
can provide support if you become ill or are injured
Cardiologists
monitor the development and severity of any heart conditions
Physical, occupational, and speech therapists
help you build strength and find easier ways to accomplish everyday tasks
Endocrinologists
can help manage diabetes, growth differences, and low bone density that result from FA
Orthopedic surgeons
can help treat scoliosis
Mental health professionals
can help you explore and cope with feelings of anxiety and depression